(Peer-Reviewed) Propensity score matching study of 325 patients with spontaneous rupture of hepatocellular carcinoma
Wei Wang 王伟 ¹, Tao Meng ¹, Ying Chen ¹, Ye-Chuan Xu 许业传 ¹, Yi-Jun Zhao 赵义军 ¹, Yan Zhang ¹, Ming-Ya Yang ¹, Zhi-Hua Zhang 张志华 ², Fan Huang 黄帆 ¹, Hong-Chuan Zhao 赵红川 ¹, Xiao-Ping Geng 耿小平 ¹, Li-Xin Zhu 朱立新 ¹
¹ Department of General Surgery, the First Affiliated Hospital of Anhui Medical University, Hefei, China
中国 合肥 安徽医科大学第一附属医院普外科
² Department of Statistics, Anhui Medical University, Hefei, China
中国 合肥 安徽医科大学 流行病与卫生统计学系
Hepatobiliary Surgery and Nutrition, 2021-06-02
Background: This study aims to find out the possible optimal therapy and assess the prognosis properly for patient with spontaneous rupture of hepatocellular carcinoma (HCC).
Methods: Propensity score matching (PSM) analysis was used to study the data from 325 patients with ruptured HCC (RHCC) and 2,291 patients with non-RHCC.
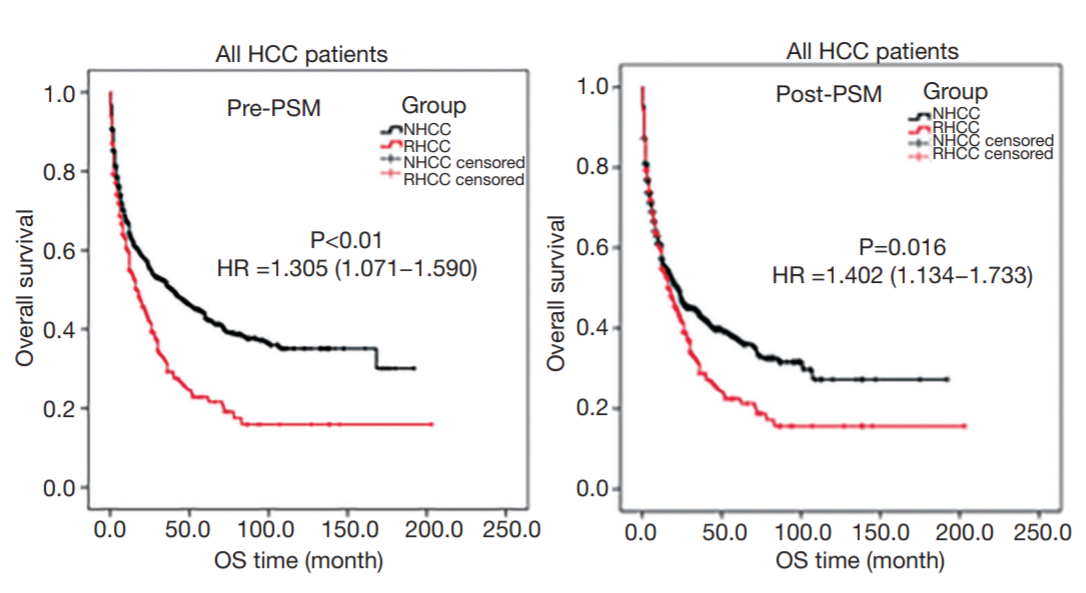
Results: The incidence and hospital mortality of RHCC were 5.1% and 0.8% respectively, with a median overall survival (OS) time of 17 months. There was no difference between ruptured and non-RHCC patients undergoing conservation treatment in terms of OS. Trans-arterial embolization (TAE) was carried out in 69 (21.2%) cases with RHCC, with a median OS of 7 months, which was no difference from that of non-RHCC (pre- and post-PSM). One hundred and sixty-nine (52.0%) RHCC cases underwent one-stage hepatectomy, with a median OS and disease-free survival (DFS) of 30 and 6 months respectively, which were shorter than that of non-RHCC (post-PSM). TAE plus two-stage hepatectomy was performed in 30 RHCC cases, with a median OS and DFS of 28 and 10 months respectively; these outcomes were better than that from RHCC patients undergoing TAE alone or one-stage hepatectomy (post-PSM), which were no difference from that of non-RHCC patients undergoing hepatectomy. The risk of death for RHCC patient undergoing one-stage hepatectomy is 1.545 times higher than that of one undergoing TAE + two-stage hepatectomy.
Conclusions: TAE plus two-stage hepatectomy might be the optimal treatment for RHCC patient. Under the premise of the same pathological properties, there is no difference in prognosis between ruptured and non-RHCC patients if the therapy is appropriate.
High-speed and large-capacity visible light communication for 6G: advances and perspectives
Nan Chi, Zhilan Lu, Fujie Li, Haoyu Zhang, Yunkai Wang, Xinyi Liu, Zhiwu Chen, Zhe Feng, Zhuoran Hu, Zhixue He, Ziwei Li, Chao Shen, Junwen Zhang
Opto-Electronic Technology
2026-03-20
Holotomography-driven learning unlocks in-silico staining of single cells in flow cytometry by avoiding fluorescence co-registration
Daniele Pirone, Giusy Giugliano, Michela Schiavo, Annalaura Montella, Martina Mugnano, Vincenza Cerbone, Maddalena Raia, Giulia Scalia Ivana Kurelac, Diego Luis Medina, Lisa Miccio Mario Capasso, Achille Iolascon, Pasquale Memmolo, Pietro Ferraro
Opto-Electronic Science
2026-02-25
A hybrid integrated high-precision tunable semiconductor laser
Yiran Zhu, Botao Fu, Zhiwei Fang, Qiyue Hu, Jianping Yu, Yunpeng Song, Yu Ma, Min Wang, Kunpeng Jia, Zhenda Xie, Ya Cheng
Opto-Electronic Advances
2026-02-12
Millisecond-level electrically switchable metalens for adaptive rotational depth mapping and diffraction-limited imaging
Yeseul Kim, Jihae Lee, Won-Sik Kim, Hyeonsu Heo, Dongmin Jeon, Beomha Yang, Xiaotong Li, Harit Keawmuang, Shiqi Hu, Young-Ki Kim, Trevon Badloe, Junsuk Rho
Opto-Electronic Advances
2026-02-12